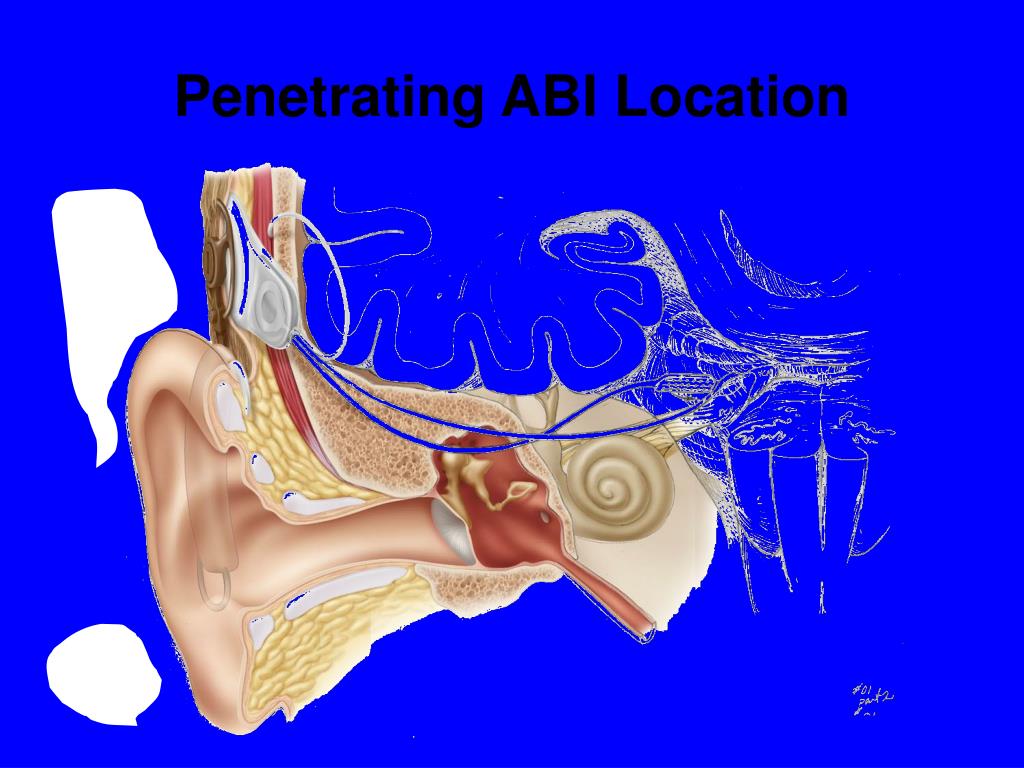
Today, multichannel cochlear implants (CI) provide access to speech, enabling many recipients to become proficient in spoken communication ( Geers, Mitchell, Warner-Czyz, Wang, & Eisenberg, 2017 Niparko et al., 2010). Implantable auditory technology has become the standard of care for children born with severe to profound sensorineural hearing loss. To date, the results indicate that spoken communication skills are slow to develop and that visual communication remains essential for post-ABI intervention. In addition, we report the scores on speech perception, speech production, and language (spoken and signed) for five children with 1–3 years of assessment post-ABI activation. In this paper, we describe the study protocol and the children who have enrolled in the study thus far. In the United States, the Food and Drug Administration has authorized a Phase I clinical trial to determine safety and feasibility of the ABI in up to 10 eligible young children who are deaf and either derived no benefit from the CI or were anatomically unable to receive a CI. However, more prospective studies are needed to confirm and further explore this potential.The auditory brainstem implant (ABI) is an auditory sensory device that is surgically placed on the cochlear nucleus of the brainstem for individuals who are deaf but unable to benefit from a cochlear implant (CI) due to anatomical abnormalities of the cochlea and/or eighth nerve, specific disease processes, or temporal bone fractures. Conclusions: Brainstem implantation has the potential to improve self-reported hearing ability, hearing-related quality of life, and reduce tinnitus in NF2 patients. 
An increase in tinnitus severity from 26 to 84 points in THI was observed in the remaining patient, who had the greatest intensity of NF2 symptoms in the postoperative period and reported the smallest benefits with ABI. Patients and was reduced in one patient (mean improvement in THI score for these patients of M = 25 SD = 21). Score of M = 38 SD = 13), which was most pronounced for basic and advanced sound perception. A considerable improvement was also noted in the patients’ hearing-related quality of life (mean improvement in NCIQ 
Based on the self-reported results, it was found thatĮach patient noticed an improvement in hearing ability (mean improvement in APHAB score of M = 25 SD = 27), which was greatest in background noise conditions. (APHAB) was used to evaluate self-perceived hearing ability and Nijmegen Cochlear Implant Questionnaire (NCIQ) to assess Results: Of the 6 patients who initially agreed to participate, 4 returned questionnaires. The Abbreviated Profile of Hearing Aid Benefit A series of 6 patients who underwent ABI in a single tertiary referral center wereĪsked to fill in two sets of questionnaires referring to their pre- and postoperative experiences. Material and Methods: The study was a retrospective design. This study evaluated the self-reported hearing ability, hearing-related quality of life, and tinnitus severity in 4 adult ABI users. One of the co-occurring symptoms in these patients is tinnitus however, little is known about its prevalenceĪnd severity. Background: Auditory brainstem implantation (ABI) is a modern method of treating hearing impairment, directed especially to patients with
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
